It is my honor and privilege to share with you our hospital’s experience in embracing digital health service in the time of the COVID-19 pandemic. First please allow me to extend my immense gratitude to the Pharmaceutical and Healthcare Association of the Philippines (PHAP), especially to Daisy Sembrano who also served as the chairman of our hospital’s multisectoral governance Council.
Our objectives are to share the actual experiences of the BGHMC regarding the use of digital processes, and to give insights on the advantages and disadvantages of digital platform in healthcare.
The shift of digitizing medicine and its health care delivery was deemed inevitable in the global scene even in the normal situation we knew in the pre-pandemic. What happened during the COVID-19 pandemic has forever changed the platform of all service delivery, all the more the healthcare services.
Before the coronavirus hit the pandemic stage, BGHMC already migrated most of its relevant processes into digital or electronic versions. It aimed to elevate the overall patient experience and lessen the voluminous processing of papers by our healthcare workers. It is an effort made by our hospital to increase efficiency and to improve health service delivery.
TERTIARY HOSPITAL
BGHMC is a Level-3 Department of Health (DOH) Hospital, located in the capital city of Balanga in the province of Bataan. There are four other government hospitals at present, eight private hospitals, with more than 200 primary healthcare facilities. Pre-pandemic, our authorized bed capacity was 264, and we had a 150% occupancy rate prior to our inclusion. Our hospital even reached 600 beds occupancy on peak seasons.
In 2017, our case mix ratio was 87% of cases admitted were primary in nature. Before this pandemic, our focus was to manage hospital congestion of primary cases in order to efficiently manage our resources intended for tertiary cases.
With the frequent surge of cases, we started to transition to the digital platform in early 2018 as we initiated the online service delivery network in Bataan. Little did we know that this will become a breakthrough process by 2019.
Our innovation was backed by our research paper that aimed to uncover why patients bypass the rural health units or district hospitals. We concluded that a functional two-way referral system must be present.
We developed an online referral system that gave birth to a province-wide linkage of health facilities to us. We aim to influence lower health facilities to properly gatekeep so that we could attend to the secondary and tertiary cases, something that our doctors and resources are specialized for and prepared to deal with. At that time, we badly needed a functional healthcare provider network in Bataan.
SDN
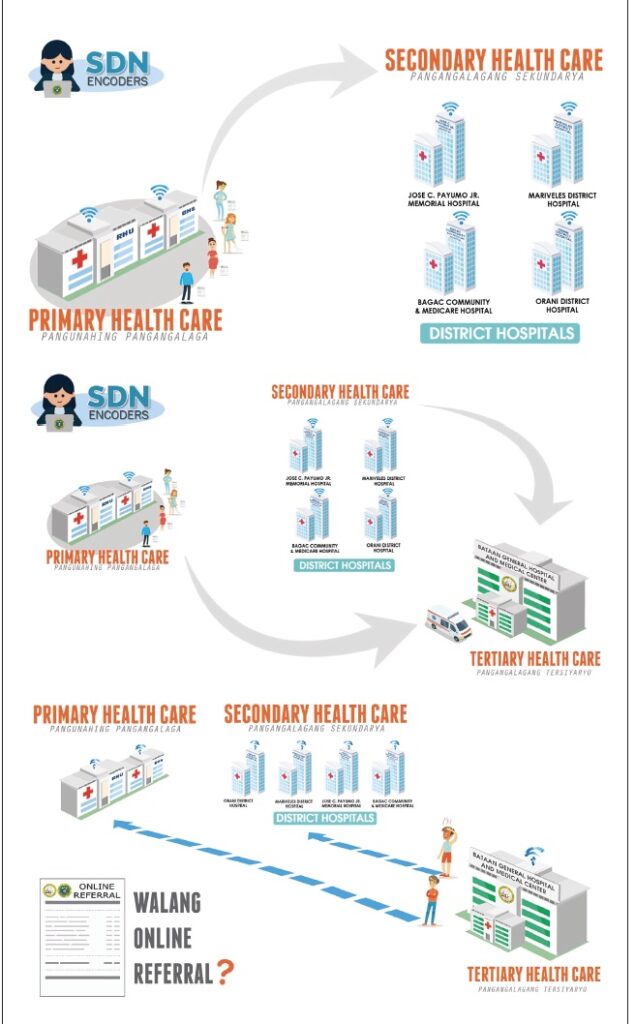
The Bataan BGHMC Service Delivery Network (SDN)-Online Referral System was initiated by coordinating with the MHO (Municipal Health Officer) and district hospital chiefs. It was not an easy task because it involved modification in the healthcare-seeking behavior of the community and commitment among primary care providers.
Ideally, members of the community must pass through their rural health unit for consultation or primary care provision. This should be a functional gatekeeping as the rural health physician or medical officers in district hospitals assess patients. They can manage or refer patients to appropriate facilities if it’s beyond their capabilities.
The two-way referral system is through an online platform powered by internet connectivity. Patients can be referred back to the lower facility for follow up and succeeding care.
Within three years of implementation, we reached the ideal case-mix occupancy rate as it started to reverse, with an 86% increase of secondary and tertiary cases in all three years of online referral system implementation.
Our online SDN experience or best practice was shared with the provinces of Aklan and Palawan, and we did technical assessment and assistance for their health service delivery. This pandemic has tested our referral system and paved the way for the version of a new software.
At the start of 2020, we focused our efforts in developing a system unknowingly appropriate to the pandemic. The online referral system now has expanded to new digital systems that became very instrumental in the efficient conduct of processes in the hospital, focusing on limited contact for consultations.
Through the online system, we have linked telemedicine to cater to our patients, the COVID-19 PCR submission of case investigation report, and the release of results. We eliminated the paper-based system and resorted to online referral. With the new version comes a whole new level of patient and user experience.
Our Out-Patient services have the SDN and the Teleconsultation. SDN is a Web-based online referral system that initially aims to decongest tertiary hospitals by organizing efficient referral from primary and secondary facilities.

TELECONSULTATION
Teleconsultation is a new addition to our electronic platform. It is a pandemic-born online registration and teleconsultation platform that minimizes face-to-face consultation between patients and healthcare workers.
Patients have to log on to the Teleconsultation—http://www.bghmc-sdn.net/telemedicine. This is communicated to the different rural health units and district hospitals, and we also post advisories on our web page and Facebook page.
In a nutshell, first, the patient has to visit the website and then that patient is required to fill in his personal information and attach a photo of a valid ID.
The information asked include full name, birthday, sex, municipality and reason for consultation. The patient will then be given a queueing number and our Family Medicine resident will triage them based on the complaint sent or registered. The medical resident of a particular department will call the patient through their registered telephone number.
EMR

An Electronic Medical Record (EMR) will be made by BGHMC doctors based on their conversation. The doctor will schedule the patient for laboratory or any diagnostic procedures as applicable. Queueing to the laboratory or imaging department are then made for the schedule of patients. Patients are apprised of the status of consultation through the online queueing.
For our In-Patient services, we have established the use of EMR, Real-Time Medicine Administration and Tracking and Bed Tracker which were born during this pandemic.
EMR is a Web-based platform that links existing medical records of patients and allows real-time access of healthcare workers to the record. The Medicine Administration and Tracking is linked to all wards including pharmacy and billing sections.
The pandemic also brought the creation of a system that utilizes real-time update of available isolation rooms through the bed tracker and beds which can be seen by lower health facilities, BGHMC healthcare workers, and the public.
Our EMR is web-based and can be viewed by our physicians using any smartphone or other digital devices as long as it is connected to the internet. It ensures protection of data privacy.
Our hospital provides tablets for the use of our physicians and desktop PCs for the nurses. If outside the BGHMC, the EMR can only be read by the healthcare worker.
Our EMR can generate a Medication and Treatment sheet that is linked to the PhilHealth’s CF-4 Form.
Our physicians are no longer struggling against other healthcare professionals to get hold of a patient’s chart in order to manually fill up the chart with history, physical exams, progress notes, checking of vital signs and monitoring of patients’ medication. The same thing holds true for nurses, pharmacists and other sections. They can all simultaneously access parts of the EMR dedicated for their inputs.
We are now working closely with PhilHealth to allow us to directly submit or upload our generated CF-4 forms through E-claims. We also provide detailed instructions from the physicians. On top of the EMR, we also incorporated a medicine tracker within the system to better track the use and management of drugs and medicines. Physicians can readily view the available drugs and medicines for their prescription. Almost all divisions are now using the EMR (Physicians, Nurse, Pharmacy, PCR Lab, Medical and Radiologic Technologists).
During this pandemic, all hospitals are facing challenges in providing treatment to patients. Due to the critical status of available beds, we developed our own bed tracker, which is linked to all wards. It can also be viewed by lower health facilities linked to our SDN. This apprises them real-time of the availability of beds. The PCR test results are being monitored for every patient as we move them to their appropriate rooms. The system also generates its own daily census.
As the most relevant digital response to this pandemic, we incorporated COVID-19 case investigation form (CIF) in our online platform, which can be filled up by all health facilities in the province for their encoding of patients’ data prior to submission of specimens.
PCR results are also released through the system. This eliminates loss of CIF and other problems related to processing of PCR requests. With the results being received in one to two days, the RESU, PESU and MESU and all facilities linked with us are apprised as we release the results.
GAINS
What are our gains? Let us look at it in terms of patient care referral system, records management, logistics management, infection transmission control, and claims and reimbursement.
For patient care, quality procedures constitute timely provision of care and ease of generating documents are made possible, such as issuance of medical certificates, medical abstract, OR technique or discharge summary.
Nurses are also provided real-time administration of medicines and carrying out of doctors’ orders. Also, it is an efficient management of time that can be monitored in the ER, laboratory, or discharging of patient, isolation room management, and referral within the hospital and outside.
Through our SDN, the following was made possible: real-time link of the primary care facilities with BGHMC, help in triaging and gatekeeping, and help in the efficient utilization of resources intended for tertiary cases. For records management, the use of the system has advantages mainly for the medical records management. Patients can request for their medical certificate through online but they should claim the actual certificate at the BGHMC on the scheduled date of claim.
The system can easily generate, store, retrieve, and dispose medical records with complete adherence to data privacy. Patients’ records, ICT-10, hospital statistics, and CF-4 is no longer a struggle for our records staff.
In terms of logistics management, it is very evident that we no longer need paper, Risograph machines, ink and maintenance and operating expenses. Gone are the days when we procure voluminous amounts of paper. During this pandemic, all of us in the field of hospital services innovates processes and systems to decrease transmission of the infection within our hospital and outside our hospital through mobile. This paperless transaction made this transmission control.
Of course, claims and reimbursements were made possible through the ease of generating essential PhilHealth documents.
Recently, our hospital became Central Luzon’s entry to the three-minute pitch to policymakers, wherein we pitched a possible policy to the concerned stakeholders for possible nationwide implementation of online referral software. We were surprisingly declared a National Champion in the Philippine National Health Research System held last August. We are currently in the stage of disseminating what our system can do today for the efficient delivery of healthcare system, and most especially to the health outcomes of the patients.
CHALLENGES
Behavior modification is a big challenge. There is a saying that you can’t teach an old dog new tricks. Simply put, when somebody’s comfort zone is altered, compliance to the change will be very difficult.
LGUs have different priorities and a short term of tenure for local executives entails a constant quest to buy-in for new ones. Logistics like hardware and software are also an issue and of course, the challenging aspect of implementing the system is basically from the grassroots of the healthcare system.
We have identified some of the healthcare workers who are challenged in using electronic gadgets, especially the senior ones. They initially saw the platform as an additional burden, which caused delays in implementing the online system in the whole province.
Challenges on the technical skills and facilities were augmented through the coordinated efforts of the LGUs together with our medical specialists as initiated in our hospital. Resources like manpower, hardware and software were also limiting factors.
Even if there was notable success in the current implementation of the BGHMC online referral system, we are still faced with more room for growth and improvement.
We are looking for ways to improve the system as we continuously aim to upgrade health facilities and expand the utilization of the online referral system software to other neighboring provinces, including specialty hospitals, to harmonize EMR with the online referral system to be accessible, also for the different rural health units for the portability of the records, to incorporate PhilHealth documents to ease generation of relevant documents for PhilHealth claims and reimbursements, and to enhance the processes for the full implementation of UHC law in the province and possibly nationwide.



